Types of Nosocomial Infections
The most important of types of nosocomial infections:
• Infection Wound Surgery
• Blood infection or sepsis
• Urinary tract infections
Infection Wound Surgery
Surgical wound infection is caused by a bacterial infection. This infection usually causes problems during or after surgery. These problems include organ damage, bloodstream infections, defects in the surgical procedure, and even death.
Common complications of this infection usually appear 5 to 10 days after surgery, but in some cases these symptoms can occur after a few weeks. The most important of these symptoms are pus and accumulation of other fluids around the sutures, pain and redness around the wound, surgery, and in some cases
Fever also noted. There are reasons for these symptoms. These causes are mainly caused by some bacteria, including streptococci, staphylococci or other microbes.
The incidence and risk of these germs is very high; So despite new pre-surgery disinfection procedures and high-level post-operative care, these infections still have a chance to occur.
Some underlying conditions in the body and characteristics of patients can make people more susceptible to this infection. For example, older people are more likely to get this type of infection than younger people. Inadequate and malnutrition, any disease, chronic, especially diabetes, use of drugs, immunosuppressants, surgery,
Gastrointestinal tract, obesity, and epilepsy can increase the risk of such infections in the hospital.
To Prevent this Infection:
- Prescribe antibiotics before surgery at the right time
• Ensure that the best possible preoperative position for the patient is selected
Use of antimicrobial solutions around the surgical incision
Use of special antibiotics, such as neomycin, before surgery in the gastrointestinal tract to sterilize the gastrointestinal tract.
• Observe sterile tips such as killing any bacteria or other microorganisms, such as viruses or parasites, around the surgical site as well as operating room equipment.
• Operating room staff use clean, sterile clothing, hats and masks• Reduce the use of stitches (use stitches, only in urgent cases)
• Clean the skin before surgery from any contamination
• Choosing the right antibiotic for the time after surgery
• Proper planning for the time and duration of antibiotics at the right dose
• Shortening the hair (instead of shaving) around the surgical incision site
• Adjust blood sugar levels to the right level in diabetics. (People with diabetes who have heart surgery need more care and attention)
Adjusting and maintaining normal body temperature in patients undergoing colon surgery.
Bloodstream Infection or Sepsis
This infection can cause shock in people. In sepsis or infection, the condition of the body is very complicated; Because the infection spreads through the blood throughout the body. During this infection, nutrients and oxygen do not reach the vital organs well. This is due to the presence of blood clots and reduction
Blood flow is created. In advanced cases, death of several organs also results from the infection. In very severe cases, a blood infection can cause a rapid drop in blood pressure. This in turn leads to infectious shock. Infectious shock is very dangerous and has harmful effects such as lung, kidney and liver failure
And eventually death. It should be noted that, blood infection is also caused by the reaction of the body’s immune system to infectious agents such as bacteria, viruses or fungi.
Some people are more likely to get the infection for underlying reasons. In general, people with severe immunosuppression are more likely to get a blood infection.
Weakened immune systems can be caused by certain diseases such as diabetes and AIDS, or even certain medications such as medications.
Chemotherapy or steroids. Cancer patients are at the forefront of the infection due to the use of strong drugs as well as people with a history of organ transplantation. Infants and children are also at risk due to the underdevelopment of their immune systems. The elderly and the sick
Diabetes is also at the risk of high-risk individuals. In general, people who have been hospitalized and have experienced intravenous injections, surgical wounds, or bed sores should pay more attention to the issue of bloodstream infection.
Causes of Blood Infection
The main cause of this disease are microbes. However, in some cases, bacteria, viruses and fungi can also be problematic. Among these, bacterial infection of the blood is one of the most common. The spread of some infections in the body, such as lung infection (pneumonia), bladder and kidney infection (urinary tract infection),
Skin infections (cellulite), abdominal infections (such as appendicitis), bone infections, and brain infections (such as meningitis) can cause bloodstream infections. In fact, postoperative infections can also cause bloodstream infections.
Who is Most Exposed to this Disease?
The elderly, as well as people taking immunosuppressive drugs, are at the forefront of the disease. For example, people who have had an organ transplant are also in this group. Patients who receive chemotherapy or radiation therapy are also at high risk.
Because the spleen is a key organ in the body to fight infections, people who have already had their spleen surgically removed should pay more attention to this.
Long-term use of steroid medications, people with AIDS, diabetes or liver cirrhosis, people with pneumonia, meningitis, cellulite (skin infection) and urinary tract infections, as well as people with severe burns and injuries to their skin Are highly susceptible to bloodstream infections.
Symptoms of a Blood Infection
Due to the fact that blood infection can occur in different organs and in different parts of the body, widespread symptoms such as rapid breathing and changes in mental state, such as decreased level of consciousness and confusion, can occur. Fever and chills, rapid heartbeat, hypotension, confusion and dizziness
Unexplained, decreased urination, nausea and vomiting, diarrhea, skin rashes and especially red rashes or red spots on the body as well as pain in the joints of the wrists, elbows, back, thighs, knees and ankles, are the main symptoms. It is considered a blood infection.
Time to See a Doctor
In many cases, seeing a doctor right away when you feel symptoms is very effective. For example, a baby who has a fever, lethargy, malnutrition, behavior change, or an abnormal skin rash and is less than two months old has an urgent need to see a doctor. In general, any occurrence
Dizziness, dizziness, palpitations, rapid breathing, fever, chills, and severe skin rash require immediate medical attention.
Ways to Diagnose a Blood Infection
In general, the main way to diagnose blood clots is to do a proper blood test. Examination of sputum, urine, spinal fluid, or abscess contents is also a must. In some cases, X-rays of the chest to check for pneumonia and a CT scan of the abdomen are also recommended.
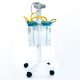
Of course, it should be borne in mind that timely vaccination of children is very effective in reducing this infection. It should be noted that patients need an oxygen mask at the time of admission and intravenous antibiotics are prescribed to the patient. Also in order to compensate for the drop in blood pressure, the doctor may use the solution
Prescribe salt or saline to the patient. In many cases, drainage surgery is recommended if there is an infection in the abdomen. Depending on the severity and effect of the bloodstream infection, kidney dialysis may be necessary.
Prevention of Blood Infection
The most important way is to prevent its occurrence. Simple adherence to hand washing and body hygiene helps prevent bloodstream infections.
Urinary Tract Infections
Typically, 5 to 10% of hospitalized patients develop a nosocomial infection. The infection affects more than 2 million people in the United States alone and kills about 88,000. It should be noted that 40 to 45% of nosocomial infections are urinary tract infections, about 80% due to the use of catheters and
About 20% get this infection due to urinary tract manipulation.
About 15 to 20% of patients get the disease through microbial contamination inside the duct. It should also be noted that the infection appears in the collection bag within 24 to 48 hours after use.
In a normal bladder, the number of germs in CC reaches 105 in 24 to 48 hours. This is while the main way of entering the urethral germ is.
Complications of Office Infection
The main complications of this infection are bacteremia, bacteremia (actually, 3.% of bacteriophages cause bacteremia), pyuria, pyelonephritis and sepsis, and multiorgan failure and death.
Prevent Urinary Tract Infections
To prevent urinary tract infection, a catheter should be used only when necessary. In fact, the aseptic method for catheterization should be observed (training method and reminding of training at intervals are recommended). Manipulation or opening of the system should be minimized and the catheter should be used only for the necessary time and the catheter should be removed as soon as possible.
Close the connections tightly when inserting the catheter. It should be noted that the use of topical antibacterials, bag disinfection and the use of catheters containing individual banners in the field of prevention has not been approved by all and it is necessary to use them only as necessary.
It is important to note that condom catheters are suitable for men without obstruction. If not followed, the risk of infection is equal to that of a catheter. Taking antibiotics in the first 4 days of catheterization also reduces infection, but increases the risk of resistant germs and fungi.
Intermittent catheterization is useful to prevent prolonged catheterization and infection and is especially recommended for young people with spinal cord injury. However, it should be noted that intermittent catheterization should never be performed in cases where trauma is possible. In general, hospital UTI treatment based on the type of germ and antibiogram culture is always sensible.





































One Response
Abadis products are of high quality and have been approved by medical centers.